"I feel like Iron Man sometimes," says Mr. Latta, who was previously working as a telecommunications contractor.
"The VAD goes in my body; it's designed, so the pump itself is in my chest and the controller and batteries go on my belt. It almost looks like I'm wearing a laptop. It weighs about five pounds and comes with two battery packs and a controller, and each battery lasts about four hours."
Morgan had his VAD installed earlier this year as part of his treatment for his congenital heart disease condition, explains his cardiac surgeon, Dr. Terrence Yau.
"The lower pumping chamber of his heart, which would normally be thick-walled, strong and capable of pumping blood out to the rest of his body, is actually in the wrong spot."
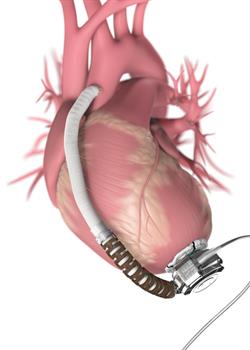
The VAD, which can fit into a person's hand, is a pump that rotates up to 10,000 revolutions per minute (how fast depends on the model). It's installed in Mr. Latta's chest, where it draws blood out of his weakened heart's pumping chamber and pumps it into a tube connected to the main artery supplying blood to the rest of his body, with another wire connecting to a controller and the battery pack.
Untreated, Mr. Latta's case would lead to a severely restricted life, "right at the time when he would normally be busy, starting a family and would expect to be physically active," Dr. Yau says.
Instead, after Mr. Latta's VAD, called a HeartWare HVAD, was installed – and his wedding took place – he was able to go home, where he waits to learn if he will be medically eligible for a heart transplant. But he can live a long time with his VAD, whether or not he has the transplant.
Mr. Latta was slated to participate in a groundbreaking international stem cell study being led by the PMCC, but had to withdraw from this because of his particular health complications. Nevertheless, he returns to the PMCC on a regular schedule to determine whether his blood pressure in his lungs has become low enough to consider a transplant. Meanwhile, he is home in Kingston, ON., with Theo and his wife.
"Once my heart rate drops and the lung pressure goes down, I can go immediately on the transplant list. I could get a new heart in a week or it could be months," he says. Many patients have VADs installed as a "bridge to candidacy" for potential transplants, Dr. Yau says.
He always gets support from the PMCC, regardless of whether he's at the centre or at home; he's in constant contact.
"Part of my role is to see patients like Morgan and their families, when they're going to get a VAD," says Marnie Rodger, Nurse Practitioner, who has expertise in mechanical cardiac assist devices.
"I meet and answer all the questions, show them the pump, the batteries, explain the surgery," she says.
"Now I'm their first point of contact. If there are problems, they call me, and our team figures out what's going on."
Mr. Latta's surgery to install his VAD was delayed due to medical complications, which is why he got married in the hospital room instead of the PMCC atrium.
There is a plus side. "I was able to train Morgan and his wife [in maintaining the device] before he actually had the VAD implanted, and that actually shortened his postoperative stay," Ms. Rodger says.
"It really does take a team, and we're very fortunate to have such a great one at the PMCC," says cardiac surgeon Dr. Vivek Rao, one of the world's leading experts on mechanical cardiac assist devices.
The technology of VADs is advancing exponentially, he adds. They cost between $80,000 and $100,000 each, and the newest versions use magnetic levitation for their high-speed internal rotation, so the rotating parts never touch each other and therefore won't wear out.
VADs boost the odds for the more than 50,000 Canadians who are diagnosed with heart failure every year, Dr. Yau says. Mr. Latta says the PMCC team and his treatment certainly have changed his outlook, too.
"At first, I was in denial. I didn't want to talk to them. Now when I come in and see them in the hallways, I talk to them as long as I can. We've become quite close."
Beyond VADs: The PMCC and the world-leading stem cell program
VADs are a medical miracle and the program at the PMCC is the largest in Canada, installing some 40 each year, performing around the same number of heart transplants. But while a VAD can keep a patient alive for many years, it doesn't improve the patient's heart function, says Dr. Yau.
He's looking for something better, through a comprehensive stem cell trial study.
"I can never take out that VAD unless I'm going to transplant you," Dr. Yau explains to Mr. Latta. "Wouldn't it be nice if we could put a VAD in and also give you stem cells that could make your heart function well enough to someday live without the VAD and the cables and without a heart transplant – just live on your own?"
The $4-million stem cell trial Dr. Yau and his PMCC colleagues are conducting is a huge study co-funded by the National Institutes of Health in the United States and the Canadian Institutes of Health Research. It's the first of its kind in the world and it's being led by the PMCC.
"It's a collaborative trial across North America, run through a network of surgical sites and surgeons, by myself and Dr. Frank Pagani, a VAD surgeon at the University of Michigan," Dr. Yau says.
Patients who take part in the study are those who receive a VAD. Doctors also implant either stem cells or a placebo in their hearts.
The doctors can turn down the patient's VAD flows to see whether the patient's own heart implanted with the stem cells shows improved function.
"We turn it down temporarily and ask, 'Do you feel okay?' " If not, the VAD gets turned back up right away. If the patient continues to feel well, with the VAD really not supporting them, the patient walks for six minutes while we measure how far they can walk, and we have several echocardiograms to assess heart function.
"This is now the second phase of the study," Dr. Yau says. In the first phase, in which a low dose of cells was used, investigators found that 20 per cent of patients who received the placebo were able to tolerate having their VADs turned down for half an hour with no ill effects.
"However, if you received the stem cells, you had a 50-per-cent chance of tolerating having the VAD turned down. That's a huge difference that we don't ordinarily see in modern medicine."
The first phase involved about 30 patients, while the second will enrol four times as many patients and is testing a much larger dose of stem cells, Dr. Yau says.
"It is by far the biggest trial that has ever been done in this population, in 15 sites across North America," he says.
"It's not the same as bringing you in and taking out your VAD, but if your own heart functions better on its own, that can only be a good thing. It's one more step toward our ultimate goal of being able to one day take out the VAD and leave the patient with their own well-functioning heart."
Geoff Speirs: Batteries and baby
As if it weren't a big enough personal breakthrough for Geoff Speirs to receive a left ventricular assist device (LVAD) and become a heart transplant candidate in 2016, another miracle came along.
Mr. Speirs, 32, became a new dad, when his son Lincoln was born in March.
"It means the world to me,"
says Mr. Speirs, who lives in Lindsay, Ont., with his wife, Dawn Rossen, 31.
"I'm living a normal lifestyle, other than having batteries and stuff," he jokes.
Mr. Speirs had been treated for heart ailments eight years earlier, when he had a defibrillator installed. Then in 2013, while working in Western Canada, he suffered a stroke and returned to Ontario.
"Those doctors are miracle workers. They told us that he was one to two days away from not making it," Ms. Rossen says.
"He was in such bad shape that it took almost two weeks to get him into shape just for the LVAD surgery."
While he waits with his LVAD for his transplant, Mr. Speirs has more energy than he did before the device was installed.
"Before, he was always tired. If we were to take a day trip to do something, for the next three days, he was out," says Ms. Rossen.
The couple like the way the medical team at the PMCC treats them. "They're nice, but they get straight to the point," Ms. Rossen says.
This may belie the enthusiasm of the PMCC team. Ms. Rodger will admit that she was "over the moon" when Mr. Speirs became a parent while on the LVAD. Like everyone else, she's impressed with the quality of life patients like him can now enjoy.
Dr. Yau says until recent years, many younger patients like Mr. Latta or Mr. Speirs might not have survived beyond childhood or adolescence; advancing medical technology and care from centres like the PMCC are changing this quickly.
"It's actually a problem that there are more cases. But it's a good problem to have," Dr. Yau says.
