
Artist Michale Payeur was diagnosed with Age-Related Macular Degeneration in 2001. Thanks to researchers at the Donald K. Johnson Eye Centre Research Institute at TWH, he was taught how to make use of an alternative visual field in order to continue to read, draw and even ride a bike. (Photo: UHN)
In 2001, Michale Payeur was about to embark on a European adventure, taking a sabbatical from his work as a designer to move to France so he could focus on art. But just before he left, he was also diagnosed with age-related macular degeneration (AMD) a progressive eye disease that damages and eventually destroys a person's central visual field.
AMD is the most common cause of vision loss in Canadians over the age of 65. The disease initially starts with distortion of lines. As it progresses vision worsens, and the patient starts to lose the ability to recognize faces, watch television and drive. The most common complaint from patients suffering from AMD, however, is the loss of their ability to read.
For an artist, it was a worrisome diagnosis.
"There wasn't much that could be done about it at the time," Payeur said. "When I got to Europe, I was monitored by doctors in Holland for the 10 years I lived there, and the disease slowly began to chew away at my eye."
Payeur's vision slowly deteriorated over the years. Although he was still able to draw, it became more challenging. Daily activities became increasingly difficult and his reading skills began to drop off.
Retraining the eye to read
Upon his return to Canada, Payeur became a patient of Dr. Michael Brent, ophthalmologist at the Donald K. Johnson Eye Centre of the Krembil Neuroscience Centre. Although nothing could be done about Payeur's lost vision, his disease could be stopped with injections to the eye, and there was also an opportunity for him to better adapt to living with AMD.
Dr. Brent referred Payeur to Drs. Martin Steinbach, Luminita Tarita-Nistor, and Esther González, researchers in the Donald K. Johnson Eye Centre Research Institute who had developed a method to help patients with AMD to see around the damage in their visual field and retain their reading skills.
In healthy eyes, a person reads by using their fovea, located in the centre of the macula in the eye's retina and responsible for sharp vision. When AMD develops, the fovea is lost and central vision is damaged, becoming either blurry or blind. Tasks where vision needs to be precise and accurate – like reading – become difficult.
Patients with AMD adapt to their loss by consistently using an area in their peripheral, healthy vision – known as the Preferred Retinal Locus (PRL) – to perform activities. Everyone's PRL is positioned slightly differently, and depending on its position on the retina, the PRL does not always allow for the best reading. Some PRL locations allow for the large visual span required for good reading, while others do not and require relocating.
However, Steinbach, Tarita-Nistor, and González's research has shown that it is possible to train patients to relocate their PRL so it is good enough to use for reading.
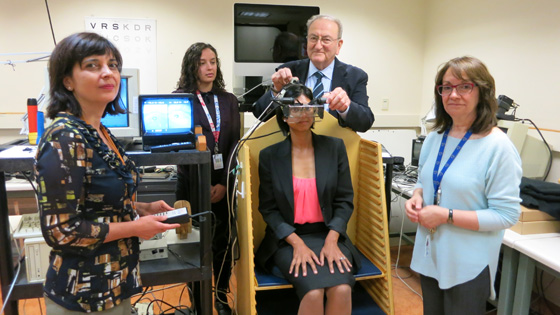
Researchers (from left) Dr. Luminita Tarita-Nistor, Taylor Brin, Dr. Martin Steinbach and Dr. Esther González use imaging technology to identify an AMD’s Preferred Retinal Locus (PRL). Once identified, the researchers will train the patient to use her PRL to read. (Photo: UHN)
Finding the 'sweet spot' for sight
With each research participant, the scientists used imaging to identify the patient's current PRL in relation to the damaged part of the eye. Next came the training.
"Patients with AMD aren't aware of their PRL and don't necessarily use the most appropriate one for reading," said Tarita-Nistor. "Through research we established how to best train patients to use a good PRL, then worked one-on-one with each of them to teach them how to make the small eye movements needed to locate this area."
Each participant attended a training session once a week for five weeks. By the end of the treatment, researchers found great improvements in the patient's eye fixation stability and the time taken to read continuous text—areas that patients struggled with as their vision deteriorated from AMD.
For Payeur, the training helped him use a good PRL that offered him a large visual span that he could use to do some of the activities he had started to have trouble with.
"This method really helped me and I now use this skill for everything," he said. "I was able to ride a bike again, I've seen improvements in my drawing and am now using a lot more colour in my art, I can still read and am able to manage all my emails. And I can do all of this despite the loss of my central vision."
Could there one day be an app for that?
Patients are currently trained to use a good PRL in one-on-one sessions in a lab setting, but researchers hope to eventually develop an app for tablets so that patients can train themselves in the comfort of their own home.
"We're very excited by this research and its future potential for patients with AMD," said Steinbach. "We are especially pleased to provide hope to patients who are suffering from vision loss."
Related Links
