
Dr. Karel terBrugge, former Head of the Division of Neuroradiology and Site Chief of Medical Imaging at Toronto Western Hospital, holds six-week old Audrey Fennell on her day of departure from SickKids Hospital in 2004, after undergoing successful complex treatment for life-threatening Vein of Galen Malformation. (Photo: Courtesy Fennell Family)
Etched in one man's legacy are the words Founding Father, President, Editor-in-Chief, Chair, Head and Site Chief. A collection of prestigious titles decorate the long and lustrous career of Dr. Karel terBrugge, who, after 40 years of clinical service and leadership with the Joint Department of Medical Imaging (JDMI), has retired from his role as Head of the Division of Neuroradiology and Site Chief of Medical Imaging at Toronto Western Hospital. (TWH)
But for 12-year old Audrey Fennell, he is simply her hero.
It was back in January 2004. Sheila Fennell had just given birth to beautiful twin girls, Audrey and Hannah. Two days later, she received the discouraging news: Audrey had been diagnosed with Vein of Galen Malformation (VGM).
This rare, life-threatening condition, which has been described as "Niagara Falls of the brain" due to the rush of blood to the brain, usually develops in utero during the embryonic stage of development, and is a result of abnormal connections between the arteries and veins in the brain.
This short circuit prevents the regulation of blood flow in the brain's blood vessels, causing an unnatural demand of blood to the brain and the push of blood into a dilated vein of Galen (a deep-draining cerebral vein). The blood in turn continuously flows back to the heart, causing the organ to become overworked and creating a great risk of heart failure for the baby.
Separated at birth
With little time to save Audrey's life, she was immediately transferred to SickKids Hospital. She weighed just four pounds. The healthcare team wanted Audrey to gain more weight before they performed surgery but within 24 hours, they realized they couldn't control the heart failure any longer.

Dr. Karel terBrugge may have stepped down from his role with the JDMI but he continues to teach and train neurointerventional therapists around the world. (Photo: UHN)
"We were told to prepare for the worst," recalls Sheila. "Dr. terBrugge informed us of the seriousness of Audrey's condition and the high risk associated with the procedure, but we had very little choice. We begged him to do everything he could to save our daughter's life – both for Audrey, and for Hannah."
To treat Audrey, Dr. terBrugge used a technique called embolization. This involves the injection of glue through a microcatheter placed directly in the brain near the malformation, which slows blood flow in the vessels and alleviates heart failure.
"Audrey's situation was extremely complex," recalls Dr. terBrugge, who retired in December 2015. "The procedure is already very risky to perform in any child, but because of her modest size and barely developed vascular system, technically it was one of the most difficult cases to treat with this type of malformation."
The level of treatment-related risk was undeniable. In 2004, survival rate for babies with VGM remained bleak. Many cases ended in death, due to the complicated nature of the treatment and the fragile state of newborns who presented with the disease. Even today, the procedure is extremely risky, with only about one third of all treatments at neonatal age resulting in a normally developing child.
The right doctor for the job
Hannah Fennell (R), 12, created this touching thank you video for Dr. Karel terBrugge, retiring Head of the Division of Neuroradiology and Site Chief of Medical Imaging at Toronto Western Hospital, on behalf of the entire family for his heroic treatment that saved twin sister Audrey’s life at just six days old. (Video: Fennell Family)
But if anyone could help save Audrey's life, it was Dr. terBrugge – the neuroradiologist who, back in the mid-1980s, helped invent a microcatheter/balloon system to treat VGM. Prior to this breakthrough, VGM was considered a "death sentence" with no existing treatment, and babies were born and died in heart failure.
Dr. terBrugge's primitive tool became the forerunner of today's standard microcatheter system that is now pivotal in the successful treatment of VGM.
Adding to his qualifications, Dr. terBrugge together with Interventional Neuroradiology pioneer Dr. Pierre Lasjaunias, were the first in Canada to successfully treat this condition in a paediatric patient in Vancouver in 1985.
There was therefore no better medical expert than Dr. terBrugge to help Audrey overcome the fight of her life.
Success at a young age
Four days after her diagnosis, Dr. terBrugge led a team of specialists to perform embolization on Audrey. Despite all odds, the procedure proved to be successful and the outcome positive with an immediate regression of the heart failure.
Only six days old and weighing just four pounds, Audrey became the smallest child in the world to undergo successful embolization of a VGM.
Now in her tween years, Audrey has some brain developmental delay as a result of the VGM, but continues to develop and grow naturally while enjoying life to the fullest.
"She is a normal, beautiful child with such a warm, generous spirit," says mom Sheila of Audrey. "She works hard every day and is able to have a normal life. There are no words to explain how grateful we are for what Dr. terBrugge has done for us and for Audrey."

Twins Audrey (L) and Hannah Fennell, now 12-years old, enjoy hanging out and skiing mountains together and say their lives would not be the same without Dr. terBrugge.
(Photo: Courtesy Fennell Family)
Defining a legacy
Pioneering the treatment for VGM that saved Audrey Fennell is one of Dr. Karel terBrugge's many career-defining achievements. From within UHN's walls to beyond Canadian borders, his global impact on the advancement of Interventional Neuroradiology (INR) has been eminent.
Simply put, Dr. terBrugge helped bring INR from a primitive pursuit into primetime clinical practice. Prior to his influence in the field, INR was associated with experimental techniques such as occluding vessels with balloons in resus monkeys. Diagnostic neuroradiology also had its limits, with only basic information available to examine disease.
"When I began in the field in the mid '70s, neuroradiology was an art," says Dr. terBrugge. "We didn't have CT or MRI imaging technology – you had to pay attention to so many details to make a diagnosis."
As part of Karel's training in the field, he was the first Fellow in Canada to learn CT scanning, later becoming a leading expert who taught this specialty all over the world.
His contributions to UHN have also had lasting effect. Dr. terBrugge came to TWH in 1976 as a diagnostic neuroradiologist. By 1987, he had built a multidisciplinary program combining the neurointerventional and neurovascular surgery teams at TWH.
This important collaboration was a first of its kind in the world, and a critical advancement in patient care. Combining the expertise of both teams – which historically functioned as independent specialties – allowed for a more thorough assessment of the patient and the right treatment option to be identified.
This joint admission between neurosurgery and INR still functions today in the TWH's AVM and Aneurysm Clinic.
This clinic, which he established together with Dr. Christopher Wallace in 1989, also provided the foundation for the TWH neurovascular database – a system that allowed the establishment of the natural history of vascular diseases in patients that had not undergone treatment for their condition.
Prior to this, it was often unknown what the risk would be if patients were left untreated with a given vascular disease. This was helpful to creating a risk management strategy where the risk of treatment could be weighed against the risk of conservative management, and helped to facilitate a new standard for treating patients.
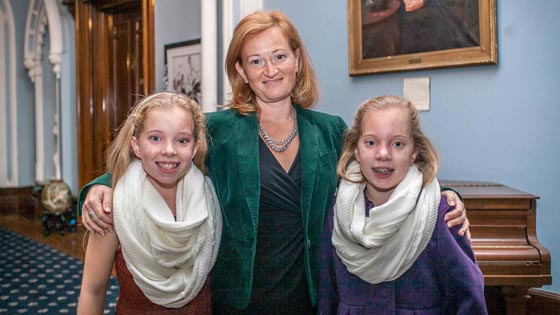
"There are no words to explain how grateful we are for what Dr. terBrugge has done for us and for Audrey," says Sheila Fennell (middle), mother of the twins, who urged Dr. terBrugge to perform the embolization procedure on Audrey at just a few days old despite its complicated risks. (Photo: Courtesy Fennell Family)
"By collecting data on the clinic's patients, we could analyze the whole picture of vascular diseases and the effects of corresponding treatments," explains Dr. terBrugge. "It allowed us to show that sometimes patients can do better without any treatment, and this indirectly saved many people from having unnecessarily risky surgeries."
With very little literature in the field at the time, Dr. terBrugge also dedicated five years of his professional life to writing, together with his colleagues Dr. Pierre Lasjaunias of Paris and Dr. Alex Berenstein from New York, a four-volume textbook that is generally considered the "ultimate handbook" used by INR professionals around the world today.
Whether through the hospital, a comprehensive database or first-rate textbooks, Dr. terBrugge has been sharing his expert knowledge around the globe for the past 40 years. He has accomplished his vision of building a world-class team of diagnostic and interventional neuroradiologists, nurses and technologists and leaves the INR team at UHN in very capable hands as he enters the next chapter of his life.
'I won't stop teaching'
Though he stepped down from his role with the JDMI last December, he continues to teach and train neurointerventional therapists around the world.
To the Fennell family's delight, this fervor doesn't appear to be slowing down any time soon.
"I won't stop teaching what I know because there are physicians in many countries around the world that need this information to look after their patients," says Dr. terBrugge. "While we may see about four to eight new vein of Galen patients per year at TWH, countries with much higher populations like India and China see a lot more of these cases and are still lacking the information and skills to manage these babies properly. They can benefit from our experience."
His vision remains very clear: "Above all else – including my own rest and relaxation – the patient has and will always come first. To me, that's exceptional patient care."
