
Drs. M. Carolina Jimenez, Allan Okrainec and Sanjeev Sockalingam, along with other members of the team, help patients on their weight loss journey with many different resources, including a new app. (Photo:UHN News)
The icon for the new bariatric self-management app is of two people climbing a mountain, one with an outstretched arm helping the other reach the top.
The symbolism is meaningful, particularly for patients who have had bariatric surgery and are in the recovery process.
"I felt I was still connected to the health-care team after surgery," says Karen Buker, Toronto Western Hospital (TWH) bariatric patient. "Often you feel abandoned and on your own but this app was very helpful."
The app was developed by the healthcare team at TWH's Bariatric Program in partnership with Seamless MD and is available for iPhone, Android and Blackberry users. The program has started a research study under the leadership of Dr. Allan Okrainec to evaluate how well the self-management app can support patients during the post-operative phase of the bariatric program.
Bariatric surgery is a procedure that changes the gastrointestinal system to help obese patients achieve weight loss. At TWH each patient is followed for five years after their surgery to lay the ground work for the lifelong changes necessary to maintain weight loss.
The app was designed to complement the other resources available to patients including support groups, cognitive behaviour therapy, and mindfulness-based therapy groups.
“Technology is a key tool to patient engagement and applications on smartphones and tablets are a simple, low cost way to helping patients achieve their health-related goals,” says Dr. Joshua Liu, CEO of Seamless MD. (Photo: Bariatric Clinic)
Daily tracking
With the advent of minimally invasive, laparoscopic surgery, patients are normally discharged from the hospital two days following their surgery.
"Patients no longer stay for lengthy periods in hospital to recover, we know that they do just as well at home and it's where they would prefer to be," says Dr. Allan Okrainec, Head of General Surgery, UHN. "We won't see that patient again for another 30 days and during that time they need to monitor their recovery, make changes to their diet and become accustomed to a new way of living – and all of this can be a lot to take in."
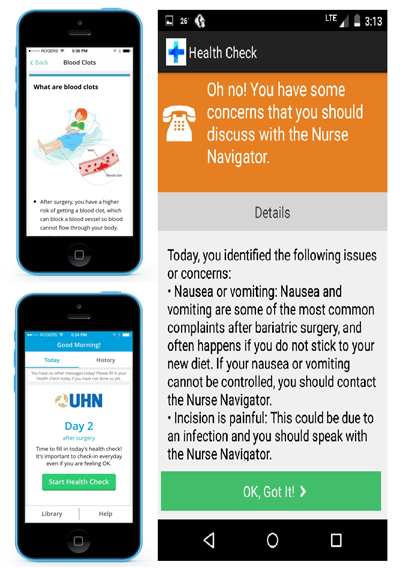
The app provides patients with the ability to track their recovery daily by indicating the symptoms they are experiencing. The information is analyzed and based on what the patient has entered, they can be directed to educational materials they can read on their own, advised to call the clinic's Nurse Navigator, or told if something is serious enough to warrant going to the emergency department.
Patients can access the online version of the Cognitive Behavioural Therapy Program and track their mood and identify triggers that might affect their eating habits. There is also a visual pill reminder service to remind themselves of the vitamins they need to take.
"When patients are better equipped to self-manage their recovery they can avoid having to come back to the hospital unnecessarily," says Dr. Sanjeev Sockalingam, Psychiatric Director of the Bariatric Program.
The app helps support patients through their journey and helps to answer questions along the way.
"With easy access to the Nurse Navigator, the app takes the guess work out of deciding if they should follow-up on something they find concerning, like pain or fever," says Mugs Zweerman, RN and Nurse Navigator for the program.
Studying the app
The study will enrol 160 patients, but with approximately 70 patients already using the app, the feedback has been very positive. According to Tim Samuel, a research assistant working in the study, all of the patients enrolled recommend that the hospital continue to provide the app following surgery.
"Healthcare teams are embracing the move for patients to become partners in their own care and supporting their ability to self-manage their own care, when possible," says Dr. M. Carolina Jimenez, a surgical resident working on the study.
