
Dr. Vera Rose, retired cardiologist (left) took care of the world’s first Mustard patient, Maria Willing (centre) for many years at the Toronto General Hospital. Cardiologist, Dr. Erwin Oechslin, Director of the Toronto Congenital Cardiac Centre at the Peter Munk Cardiac Centre now oversees her care. (Photo: Maria Willing)
There is little doubt that throughout her life, Maria Willing has lived up to her name.
Born with "blue baby syndrome," Maria was given six months to live. The syndrome is also known as the transposition of the great arteries - a form of cyanotic heart disease where the pulmonary and systemic circulation run parallel instead of in series resulting in a low blood-oxygen level. She had two holes made into her heart at only three weeks of age to allow mixing of the blue (non-oxygenated) and pink (oxygenated) blood.
At that time, blue babies had a less than 20 per cent survival rate, but Maria defied all odds and continued to grow stronger. By 18 months, she was given the green light to be the first baby to undergo a new surgical procedure – a heroic repair to the transposition of the great arteries – performed by Dr. William Mustard at the Hospital for Sick Children in Toronto.
A Mustard baby
On May 16, 1963, Maria made medical history and became the poster girl for the groundbreaking surgical procedure, which came to be known around the world as the Mustard Procedure.
The Mustard Procedure allows oxygenation of the blood in the lungs. By 1987, the procedure had saved more than 500 babies at the Hospital for Sick Children and thousands worldwide. Survival to adulthood increased to 80 per cent and these babies became known as "Mustard babies."
Over the years, the hospital had lost touch with Maria – her family lived in Whitby and later moved to Renfrew. It wasn't until she was 30 years old, facing another complication, that she was drawn back to Toronto. She had developed atrial fibrillation and experienced irregular heart rhythms. She knew something was terribly wrong.
Related to this story:
Maria vividly recalls sitting in her kitchen in Renfrew surrounded by the cupboards she had painted blue: "I just sat there thinking 'I'm going to die.'"
But she wasn't willing to give up. Feeling she had nowhere to turn, she called the Hospital for Sick Children in Toronto. "I told them I had the Mustard procedure done and they immediately said, 'Can you get here tomorrow?'" Maria drove all the way to Toronto only to realize that they were referring to the nearest children's hospital – the Children's Hospital of Eastern Ontario in Ottawa.
The wrong way, the right choice
"I went the wrong way but made the right choice," said Maria. That fateful choice brought her to Toronto General Hospital. "They saw me at Sick Kid's and immediately referred me to Dr. Peter McLaughlin at Toronto General Hospital."
Circumstances became so bad that she had to be cardioverted three times. The process involved converting an abnormally fast heart rate or arrhythmia to a normal rhythm through electricity or medication.
Then – she had a stroke. The doctors acted fast and within a week, she was fitted with a pacemaker.
Maria attributes her survival to the fine work of the doctors at the Toronto General Hospital who gave her a second chance at life. Now 53 years old, she attends annual follow-ups at the Toronto Congenital Cardiac Centre at the Peter Munk Cardiac Centre. "I always take a few days off and go on a mini-vacation to Toronto with my girlfriends," said Maria.
Over the years, Maria has developed a strong relationship with her former cardiologist, Dr. Vera Rose, who retired two years ago. Now, she is under the care of Dr. Erwin Oechslin, Director of the Toronto Congenital Cardiac Centre.
"We have a good rapport," Maria says. "The joke is [Dr. Oechslin] always wants me to have the stress test and I always refuse." Maria believes that although she has developed "a great deal of anxiety" stemming from the surgeries she experienced as a baby, she has also developed a realistic understanding of her well-being.
"We see Maria once a year to monitor her heart function and heart rhythm," Dr. Oechslin says. "Her lifestyle is healthy, she is physically active, and watches her diet and her weight. She also has good genes."
In 2001, Maria was selected to speak at an annual cardiac conference where she thanked the late Dr. William Mustard and the care she received at Toronto General Hospital and the Hospital for Sick Children.
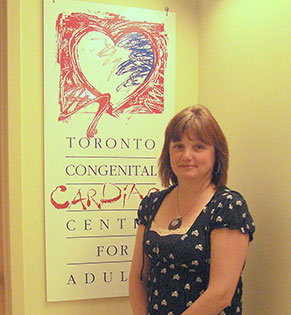
Maria is a Mustard baby, but her youthfulness makes it difficult for some to believe that she made medical history. (Photo: Maria Willing)
Feeling truly blessed
Maria continues to amaze the medical profession. A mother of three, she once recalled waiting in the hospital to undergo cardiac catheterization.
She watched as a young Fellow darted in and out of the waiting room. Finally he stopped in front of her and said "You're Maria?" looking flabbergasted. "You don't look like a Mustard baby." Maria laughed and said he was expecting to see a much older-looking woman.
Today, Maria and her husband, Brad Willing, own a marina in Haliburton. Open from April to the end of October, Maria manages a busy convenience store situated in the marina.
She attributes her youthfulness to the careful attention she pays to maintaining her health. "Last year, I got sick and I thought I was going to have a heart attack," she said. "I didn't want to take the chance so we hired someone to help out."
During the summer, Maria and her husband often sneak in an evening cruise aboard their favourite pontoon. They call it a "snoopy cruise" and glide over the lake to take in the tranquility just before sundown.
"I like the calmness the water makes me feel," she said. "I have all the time in the world to enjoy the water. We are truly blessed."
DID YOU KNOW?
In the 1980s, the Mustard Procedure was replaced by the Jatene procedure, the arterial switch procedure to repair complete transposition of the great arteries. All survivors of the Mustard or Jatene procedure – like all patients born with congenital heart disease of moderate or great complexity – had to be transferred to Adult Congenital Heart Disease Centres with special expertise.
According to Dr. Oechslin, "patients with a Mustard Procedure are at risk for long-term complications and require long-term follow-up in a specialized centre. 50 per cent of patients with a Mustard procedure who graduated from the Hospital for Sick Children are not associated with an Adult Congenital Heart Disease Program and are lost to follow-up – we don't know where they are and how they are doing. Only an emergency brings some of them back to the health care system."
