About first rib resection surgery
The First Rib Resection is a decompression surgery for Thoracic Outlet Syndrome. The surgery is to help relieve pain felt in the arm or hand, or to reduce the risk of having a further upper arm venous clot.
Pressure on the blood vessels or nerves that supply blood to your arm and hand can cause blood flow issues or nerve damage. To relieve the pain, your surgeon will remove the first rib, certain muscles or surrounding tendons and fibrous bands that were pressing on the vessels and nerves.
Before my first rib resection
Pre-Admission Visit
You will have an appointment at the
Pre-Admission Clinic within 2 weeks before your operation. This visit is very important to assess your health and help you prepare for your surgery and recovery. Plan for your visit to take 2 to 5 hours. On the day of your pre-admission visit, take your medications and eat as usual, unless you were given other instructions.
What should I bring to my pre-admission appointment?
- Your health card (OHIP card). If you do not have an OHIP card, please bring another form of government-issued photo ID, such as a driver's license or passport.
- Any other insurance cards. You will need the policy number of your extended health insurance, if you have any.
- Your spouse/partner, a trusted friend or family member (to offer you support and be a second set of ears).
- All the medications you take in their original containers. This includes prescription medications, over-the-counter medicines, vitamins, supplements and herbal or natural products.
- A copy of your power of attorney for personal care and/or advanced directives.
- A list of any questions that you may have about the operation and recovery.
- The name or phone number of your pharmacy, as well as any medical specialists that you have seen in the past 3 years.
- If you have had a cardiac stress test, echocardiogram and/or a pulmonary function test in the past 3 years, it would be helpful to bring a copy of the final report with you to this appointment.
What happens during my pre-admission visit?
- You will have blood tests and routine skin swabs. The swabs are taken from your nose and other areas of your body to check for germs that can cause infections.
- You may also need an
electrocardiogram (ECG) to check your heart and a chest
x-ray to check your lungs.
- You will meet many health care providers during your pre-admission visit. Please feel free to ask them any questions that you may have.
- A pre-admission nurse will review your health history and give you information to prepare you for your operation, including directions for cleaning your skin, eating before your operation, taking your medications and pain management.
- A pharmacist will review your medications.
Depending on your needs, you may also meet:
- An anesthetist who will review your health history, discuss your anesthetic plan and pain relief after your operation.
- A member of the medicine team, if you have other complex health problems.
Preparing for my first rib resection
The day before your surgery
- Do not eat or drink after midnight on the night before your operation.
Stop smoking before your surgery: learn how smoking and tobacco can affect your recovery after surgery, and how
quitting can improve your health.
What Should I do the day of my surgery
Arrive 2 hours before your scheduled operation time.
Surgical Admission Unit (SAU) at
Toronto General Hospital
Peter Munk Building – 2nd Floor
All hospital entrances are open by 6:00 am. However, Elizabeth St. and University Ave. are easiest to access.
After my surgery
You will stay in the
Post Anesthesia Care Unit (PACU) for a few hours. After you have recovered, you will be moved to the
Vascular Surgical Inpatient Unit.
What can I expect to have on my body?
You will be attached to some or all of these machines and tubes:
| Incisions, tubes or drains | What to expect |
|---|
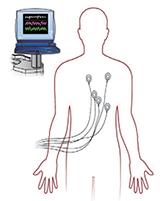
|
Heart monitor: You will be on a heart monitor while you are in the Step Down Unit. |
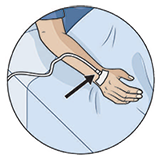
|
Intravenous (IV): You have an IV so we can give you fluids and medicines. It stays in until you are drinking well. |
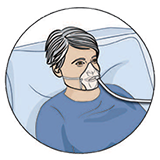
|
Oxygen: You may need oxygen after your surgery. At first, you will have an oxygen mask over your nose and mouth. When you no longer need the mask, you may get oxygen through your nostrils (nasal prongs). |
Back at home
| Activity | How to manage at home |
|---|

| - Follow the medication instructions in your discharge summary. You can take your regular medications as usual, unless you were given other instructions. It is important to take your medications as directed, to stay healthy and keep your stent graft open.
|

| - You may resume your usual diet, unless you were given other instructions.
- Lack of appetite is very common and takes a few days to improve.
- IMPORTANT: Drink a lot of fluids for at least one week after your operation (unless your doctor has told you to restrict fluids).
|

| - It is normal to pass a lot of urine after your operation. This is your body's way of getting rid of the extra fluids you were given during your operation.
- Some pain medications can cause constipation (fewer bowel movements, or bowel movements that are hard and difficult to pass). To prevent constipation, drink lots of fluids (unless your doctor has told you to restrict fluids) and eat foods with lots of fibre such fruits, vegetables and whole grain breads. Prunes or prune juice can also help prevent or relieve constipation.
- If you have constipation, use a laxative such as Senokot® If you need help to choose a laxative, talk with your pharmacist. Avoid excessive straining when you have a bowel movement.
|

| - You can have a shower 2 or 3 days after surgery.
- Gently wash your incision with soap and water. Rinse well and pat dry with a clean towel.
|

| - Avoid any heavy lifting or strenuous exercise for a month after the operation.
|

| - Do NOT lift, push, or pull anything with either hand that is over 5 pounds for up to 4 weeks.
|

| - You may drive a car in 3 to 4 weeks after you check with your family doctor.
|

| - If you needed a chest tube after surgery, do not fly for 4 weeks.
|
Follow-up appointments
Where and when
2 weeks after your operation, you will have an appointment at the
Vascular Clinic. You will have another appointment about 3 months after the operation.
