Your surgeon has recommended Endovascular Aneurysm Repair (EVAR) to treat your aneurysm. There are 3 types of EVAR. The type of operation you have will depend on the location and nature of your aneurysm:
Endovascular aneurysm repair (EVAR) is repair of an abdominal aortic aneurysm and/or iliac aortic aneurysm.
Thoracic endovascular aneurysm repair (TEVAR) is repair of a thoracic aneurysm.
Advanced EVAR requires repair of a thoracoabdominal aortic aneurysm, or one close to the kidney arteries, often using a custom-made graft with branches or openings (fenestrations) to re-attach important arteries of the thoracic and/or the abdominal aorta.
Pre-Admission Visit
You will have an appointment at the Pre-Admission Clinic within 2 weeks before your operation. This visit is very important to assess your health and help you prepare for your surgery and recovery. Plan for your visit to take 2 to 5 hours. On the day of your pre-admission visit, take your medications and eat as usual, unless you were given other instructions.
What should I bring to my pre-admission appointment?
- Your health card (OHIP card). If you do not have an OHIP card, please bring another form of government-issued photo ID, such as a driver's license or passport.
- Any other insurance cards. You will need the policy number of your extended health insurance, if you have any.
- Your spouse/partner, a trusted friend or family member (to offer you support and be a second set of ears).
- All the medications you take in their original containers. This includes prescription medications, over-the-counter medicines, vitamins, supplements and herbal or natural products.
- A copy of your power of attorney for personal care and/or advanced directives.
- A list of any questions that you may have about the operation and recovery.
- The name or phone number of your pharmacy, as well as any medical specialists that you have seen in the past 3 years.
- If you have had a cardiac stress test, echocardiogram and/or a pulmonary function test in the past 3 years, it would be helpful to bring a copy of the final report with you to this appointment.
What happens during my pre-admission visit?
- You will have blood tests and routine skin swabs. The swabs are taken from your nose and other areas of your body to check for germs that can cause infections.
- You may also need an
electrocardiogram (ECG) to check your heart and a chest
x-ray to check your lungs.
- You will meet many health care providers during your pre-admission visit. Please feel free to ask them any questions that you may have.
- A pre-admission nurse will review your health history and give you information to prepare you for your operation, including directions for cleaning your skin, eating before your operation, taking your medications and pain management.
- A pharmacist will review your medications.
Depending on your needs, you may also meet:
- An anesthetist who will review your health history, discuss your anesthetic plan and pain relief after your operation.
- A member of the medicine team, if you have other complex health problems.
Stop smoking before your surgery: learn how smoking and tobacco can affect your recovery after surgery, and how
quitting can improve your health.
What Should I do the day of my surgery
Arrive 2 hours before your scheduled operation time.
Surgical Admission Unit (SAU) at
Toronto General Hospital
Peter Munk Building – 2nd Floor
All hospital entrances are open by 6:00 am. However, Elizabeth St. and University Ave. are easiest to access.
You will stay in the Post Anesthesia Care Unit (PACU) for a few hours. After you have recovered, you will be moved to the Cardiovascular Intensive Care Unit (CVICU). Your nurse will closely monitor your health until you are ready to be discharged or transferred to the Vascular Surgical Inpatient Unit.
What can I expect to have on my body?
You will be attached to some or all of these machines and tubes:
| Incisions, tubes or drains | What to expect |
|---|
|
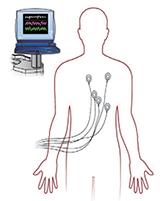
Heart monitor: You will be on a heart monitor while you are in the Step Down Unit. |
|
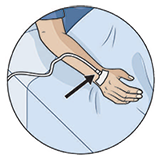
Intravenous (IV): You have an IV so we can give you fluids and medicines. It stays in until you are drinking well. |
|
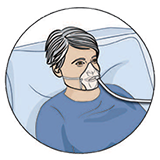
Oxygen: You may need oxygen after your surgery. At first, you will have an oxygen mask over your nose and mouth. When you no longer need the mask, you may get oxygen through your nostrils (nasal prongs). |
|
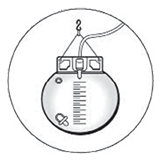
Urinary catheter: You will have a tube draining your bladder overnight. |
Where and when
All follow-up is done by your family doctor and/or your surgeon. We will try to give you a schedule of all your follow-up appointments (or mail it to you) right after your discharge or clinic visit. If you do not know your next appointment, please call your surgeon's office.
To make or change appointments, call your surgeon's office.
Your surgeon strongly recommends that you make a commitment to lifelong follow-up of your stent graft. Your graft should be checked regularly every 6 to 12 months.
