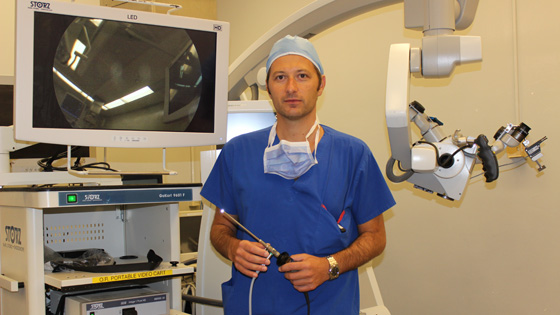
Dr. Ivan Radovanovic, neurosurgeon, holds an endoscope – an instrument with a camera on the end that is inserted in a small opening in the skull to transmit images from inside the brain to the screen on the left.
In a world first, he relied solely on the endoscope to clip a patient's aneurysm. Since endoscopes only require a small incision to access the inside of the skull, Dr. Radovanovic didn't need to use the larger surgical microscope (right) traditionally used for this procedure. (Photo: UHN)
How is it possible to make brain surgery less invasive when treating an aneurysm?
For patients with unruptured aneurysms in certain parts of the brain, the procedure to remove them involves major surgery. Doctors must make a large hole in the skull in order to reach the aneurysm which exposes the brain for a long period of time, causes longer recovery time for the opening to heal and can leave substantial scars.
Aneurysms occur when an area of a blood vessel starts to fill with blood causing a bulge in the wall of the vessel. As an aneurysm increases in size, so does its potential to rupture or burst causing bleeding in that part of the body which, in some cases, can lead to death. In neurosurgery, to treat aneurysms in the brain, surgeons remove a bone flap from the skull to access the brain and close the neck of the artery feeding the aneurysm with a clip.
"Other procedures in neurosurgery, such as those for some brain tumours, have found ways to treat the problem with the aid of an endoscope, a tube-like instrument with a camera on the end that is inserted in a small opening in the skull to transmit images from inside the brain. This allows operating through very small incisions and small bone openings and I was motivated to see if I could refine these techniques for brain aneurysms," said Dr. Ivan Radovanovic, neurosurgeon at the Krembil Neuroscience Centre (KNC). "Could I develop a method that would not only be less invasive, but still allow access to the brain for the most effective treatment?"
Performing the world's first endoscopic procedure
On May 21, 2014, Radovanovic performed the world's first small-incision procedure for aneurysms done entirely with the help of an endoscope, reducing the incision and the skull flap normally made to access the brain to less than a third of the usual size: from an eight centimetres by six centimetres opening to one of only two by two centimetres.
Since the endoscope is so thin with a camera embedded at the end, Radovanovic reasoned he could use this instrument as his "eyes" to locate the aneurysm in the brain and clip it with his surgical tools as he viewed the images of the bulging blood vessel from the endoscope on a screen.
After practicing the technique in the anatomy lab, Radovanovic felt confident to bring it to patients in the operating room.
Almost a year ago, Carmela Sosa Fernandez, 59, had an aneurysm rupture causing bleeding in her brain. It was successfully treated, but doctors also detected a second aneurysm that needed treatment.
Small aneurysms have a low chance of bleeding and do not always require treatment, but the location of the aneurysm and the fact Fernandez had already experienced a bleed put her in a higher risk category for this aneurysm to rupture as well.
Since it was a small aneurysm in a favourable location in the brain to try his new approach, Radovanovic suggested his new surgical technique for Fernandez to consider.
"I was more scared of the thought of having my skull opened than for Dr. Radovanovic to try his method," said Fernandez. "So when he explained it would be less invasive and allow for faster recovery, I had no problems with letting him test it on me."
With the help of Dr. Michael Tymianski, head of neurosurgery at UHN, Radovanovic performed the surgery, relying only on an endoscope to find and clip the aneurysm in Fernandez' brain. The procedure was successful and Fernandez was able to go home after a one night stay at TWH. When traditional techniques are used, patients usually stay in the hospital between three and seven days.
"Minimally-invasive aneurysm surgery has been practiced at UHN since 2007, and has benefited hundreds of patients," said Tymianski. "Now, with the addition of leading-edge endoscopic techniques, Dr. Radovanovic has pushed the envelope even further, making the surgeries even less invasive and potentially even less disruptive for patients' lives. This first-ever use of an endoscopic technique to treat a brain aneurysm represents our continuing commitment to providing our patients with the best and most advanced care possible."

Carmela Sosa Fernandez (right) and her husband. Carmela agreed to be the first case for Dr. Radovanovic new surgical method to treat brain aneurysms. (Photo: Carmela Sosa Fernandez)
Helping the patients of the future
Speaking from her home in North York two weeks after the surgery, Fernandez hasn't experienced any headaches or dizziness and couldn't be happier with her choice to try this new method.
"It's exciting to think that I am part of this next frontier for patients," she said. "Just like research for cancer, we need developments in procedures that will help patients have a faster recovery. This new method is great for the future."
Once fully recovered, she will only have a two inch scar behind her hairline as indication that she had brain surgery, much smaller than the six to eight inch scars usually left through the traditional method of opening the skull.
Radovanovic hopes to continue to refine the method to the point that the incision becomes the size of a pinhole. He is also interested in seeing how this approach might be applied to treat other conditions at the base of the skull and in the brain.
"I am very encouraged by the possibilities for this method and happy to have made this contribution to my field," he said. "But ultimately, being able to improve this procedure for patients is really the best outcome of this success."
Related Links
