UHN is celebrating Heart Month with courageous stories of the heart. Thanks to patients from The Peter Munk Cardiac Centre and Toronto Rehab's Cardiac Rehab program for sharing them with us.

In 2011, when Dave Allingham was rushed to Toronto General Hospital, he not only feared for his failing heart, but that he might never see his kids again.
Family was paramount to the 41-year-old father of two, who worked for a manufacturing company in Cambridge, Ont.
Dave's own father passed away of an unknown heart condition at 36. The worry of leaving his own children at such a young age was always close to mind.
"My mother used to say, 'You've got the Allingham heart'," recalled Dave. "And I did everything I could in life to keep myself healthy."
But there was only so much he could do to fight family history.
Genetic heart condition
In 2004, Dave was diagnosed with Arrhythmogenic Right Ventricular Dysplasia (ARVD). ARVD is a genetic heart condition causing abnormal heart rhythms.
Years earlier, doctors told Dave that a "swollen heart" had caused his dad's death.
"But then I finally knew what his real diagnosis was," Dave recalled.
'Felt crummy'
One day shortly after Dave was diagnosed, something didn't feel right.
He was 34 at the time— only two years younger than Dave's father was when he died. Feeling "crummy", Dave drove himself to a a nearby hospital and stayed there for the next two weeks.
His care team implanted Dave with a defibrillator and gave him a multitude of medications.
"For the most part, the drugs were well-managed and worked for me," said Dave. "I was able to go back to work at the manufacturing office for three or four years before the defibrillator started giving me some shocks."
Dave was treated with four separate cardiac ablations– a process where small areas of the heart are intentionally destroyed to improve heart rhythm.
They didn't help.
'Dire' situation
In 2011, Dave was told that he needed a heart transplant.
He was rushed to Toronto General Hospital and placed on the transplant list.
"Dave's situation was so dire that he needed life-support in Hamilton just to get him here to Toronto," said Dr. Vivek Rao, Head, Cardiovascular Surgery, Peter Munk Cardiac Centre. "Once here, we could provide advanced support and keep him alive long enough to find a donor heart."
Mechanical heart
Support came in the form of a mechanical heart, called a BiVAD (biventricular assist device). Occasionally referred to as the CentriMag system, BiVAD does the pumping for the patient's failing heart. The Peter Munk Cardiac Centre is one of only two centres in Ontario capable of providing adult BiVAD support.
"The risk to putting a patient on a BiVAD, unlike smaller assist devices and implantable mechanical hearts, is that a patient can only stay on this support a short time before their blood starts to clot," said Dr. Terrance Yau, the cardiothoracic surgeon who performed Dave's BiVAD surgery. "Once we connected Dave to the BiVAD, the transplant countdown clock would begin ticking."
"I'd been in-and-out of the hospital regularly for years and my mentality was 'get the medication and get out of here'," said Dave. "But I knew that when I hit The Peter Munk Cardiac Centre, I was in the best place I could be. There was nothing more that I could do at that moment. Whatever was going to happen was out of my hands and in the hands of my surgical team and faith."
'Dad is strong'
Dave's kids, Cole, 12, and Brittany, 14, were in Hamilton and he knew that, despite being with Canada's preeminent surgical team for his BiVAD, the procedure had risks.
The day of the BiVAD surgery, Dave asked for his kids to come to Toronto to see him, "possibly for the last time," said an emotional Dave. "When they came I hugged them and told them that 'Dad is strong. He's going to get through this and he's not going to let it beat him.' But it was a real low because I didn't know if I'd be waking up."
Waiting for a donor
Dave survived the BiVAD surgery. While the machine pumped for his heart, the countdown for a suitable heart continued.
"I became very aware of how precious time can be," he said.
While on the BiVAD, Dave was confined to the hospital and monitored very closely. He was awake, off traditional life-support and walking short distances in the unit.
'Medical miracle'
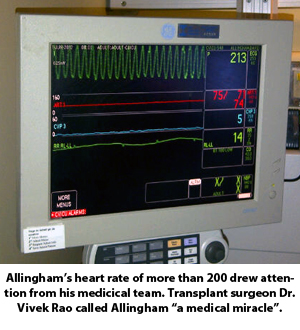
Dave's care team was fascinated by him. His heart rate often exceeded 250 beats per minute but, remarkably, Dave was feeling well and could engage in conversation. It was so astounding that Dr. Rao even took photos of Dave's heart rate monitor.
"It's a medical miracle that a patient with a cardiac arrhythmia and heart rate of more than 200 is alive and talking while his heart is essentially non-functional," said Dr. Rao.
Dave attributes his success to the power of positive thinking.
"I faced a lot of moments when I didn't think I'd make it," Dave remembered. "So I felt there had to be a reason I'd come this far. And that gave me the faith that I'd make it."
Donor heart
Finally, after two weeks of being on BiVAD, Dave was told a heart was available. Dave was able to call his wife, Paula, who had stood by him through the entire ordeal, to tell her he had a new heart.
"It was a gift that money couldn't buy," said Dave. "Even in the midst of their loss, someone's family gave their loved one's heart to a stranger and that heart gave my children their father back."
"I'll never be able to thank them for that gift," he continued.

Giving back
Dave's now dedicated himself to helping others find that same joy.
He started small, with a poker night among his friends from work.
"I wasn't being preachy but as the topic of my transplant came up, I mentioned the organ donor shortage in Ontario and Canada," said Dave. "They had no idea how few people are registered as organ donors and how many Canadians will die on a waiting list."
The next day, three of Dave's friends told him they'd registered as organ donors at
beadonor.ca.
He was so touched, it encouraged him to do more.
That's when he joined Heart Links, a support group comprised of Peter Munk Cardiac Centre heart transplant patients. They work as patient advocates increasing awareness and registrations for organ donation.
Healthy for the first time in years, Dave is eager to spend his newfound energy helping others find a donor.
With his new Allingham heart, he's not slowing down.
Dave will be joining the Heart Links group on Valentine's Day, Feb. 14, at Toronto General Hospital as they show their appreciation for Peter Munk Cardiac Centre staff at one of their annual events.
It'll be a very busy Valentine's Day for Dave because he'll also be attending the Toronto General & Western Hospital Foundation's
Heart in the City
event at Yonge-Dundas Square.
More Heart Month stories:
