
On Jan. 21, Gurdip Bhatia and his wife, Jasraj, celebrated their 40th wedding anniversary, the very same day that Gurdip became one of the longest-surviving Canadians on a mechanical heart, marking five years with a Left Ventricular Assist Device (LVAD). (Photo: Peter Munk Cardiac Centre)
 Gurdip Bhatia is one of Canada's longest surviving patients with a mechanical heart.
Gurdip Bhatia is one of Canada's longest surviving patients with a mechanical heart.
And it almost didn't happen.
"I was told by Dr. (Vivek) Rao that I'm going to need a mechanical heart and he said I'm going to carry this device 24/7 and I was kind of scared." Bhatia, who is also a cancer survivor, told CTV's Canada AM during an interview marking his five-year anniversary with a Left Ventricular Assist Device (LVAD).
"I did not (at first want to) give any consent. But my kids, you know my daughter and son, they started crying. 'Dad we need you. Dad don't you want to see our weddings, don't you want to see your grandchildren?'"

(L to R) CTV Canada AM host, Marci Ien, along with Jasraj and Gurdip Bhatia, and Dr. Vivek Rao, a cardiac surgeon at Peter Munk Cardiac Centre (PMCC), following an appearance on the national morning show discussing Gurdip's fifth year anniversary with a mechanical heart. (Photo: PMCC)
Related to this story:
LIFE-SAVING INNOVATION
HARROWING MEDICAL JOURNEY:
His zest for life is emblazoned across his face – shining through in bright, gentle eyes and evidenced by a warm, broad smile that envelopes those he meets. All of which makes it almost impossible to imagine the ordeal that Gurdip Bhatia and his family have endured.
2001 – First heart attack
2002 – Diagnosed with congestive heart failure
2003 – Second heart attack
2007 – Fitted with a defibrillator. Procedure performed by Dr. Vijay Chauhan, a cardiologist at the Peter Munk Cardiac Centre
2007 – Cardiac arrest
2010 – Collapsed on his son's wedding day – taken by ambulance to the hospital prior to the ceremony
2011 – Implanted with a LVAD in a procedure performed by Dr. Rao
2011 – Suffered a mini stroke, severe rectal bleeding, appendicitis twice, with it removed the second time
"They said your life expectancy could be two days, two weeks, two months. This changed everything," says Bhatia.
The 'this' is a battery pack slung neatly over his shoulder in a black bag. It powers his mechanical heart. The battery pack is connected to a drive line on one end, and to a Heart Ware device (mechanical heart) that is surgically implanted onto his heart at the other end.
The drive line is pierced through the skin, acting like a power cord that connects the device to the battery pack that keeps it running.
"At the time that Gurdip had his device, the primary goal was to put a device in and keep them alive until a donor heart became available," says Dr. Vivek Rao a cardiac surgeon at PMCC who performed Bhatia's surgery. "People like Gurdip have proven to us that you don't need to necessarily have a transplant to enjoy the benefit of these devices.
"As a result we've been now offering these types of devices to patients who are otherwise not candidates for transplant and have given them a new lease on life."
MAKING HISTORY
At five years, Bhatia is the second longest-surviving patient with a mechanical heart at PMCC, and among only a handful in Canada.
"Five years is significant for our program as only a few patients have been supported that long," says Dr. Rao. "I continue to be amazed at the engineering technology that allows a metal pump to function so well in the human body for so many years."
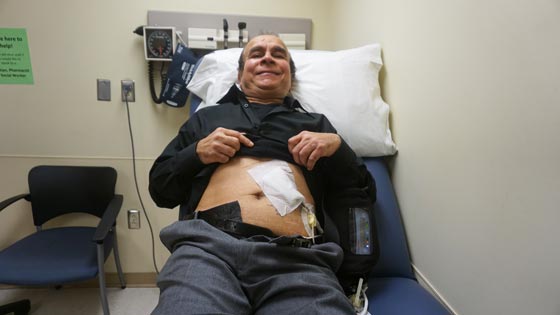
Gurdip Bhatia, heart failure patient at PMCC, during a clinic visit on the fifth anniversary of his mechanical heart surgery, displays the drive line that connects his artificial heart, or LVAD, from inside his body to the outside, powered by a battery pack shown in a black pouch. (Photo: PMCC)

Members of Gurdip’s Bhatia’s heart failure care team at the Peter Munk Cardiac Centre include: Nurse Practitioner Marnie Rodger and Mike Walker, an Exercise Physiologist, (middle) and Gurdip’s wife, Jasraj Bhatia. (Photo: PMCC)
MODERN-DAY MECHANICAL MIRACLE
DID YOU KNOW?
The Peter Munk Cardiac Centre is a global leader in expertise involving cardiac-assist device technology, a.k.a. mechanical or artificial hearts.
In 2014, the next-generation of mechanical hearts, the HeartMate III, was implanted by Dr. Rao and his team into the first Canadian patient.
Read his story ».
152 – Total number of ventricular assist devices (VADs) implanted at PMCC since program began in 2001
149 – Number of Left Ventricular Assist Devices (LVADs) implanted
3 – Number of Right Ventricular Assist Devices (RVADs) implanted
2001 – Mechanical cardiac-assist device technology program is introduced at PMCC
2011 – 100th patient implanted with a VAD at PMCC
2016 – 200th patient will be implanted with a VAD at PMCC
Marnie Rodger, a Nurse Practitioner at PMCC, has been part of the multi-disciplinary team involved in Bhatia's care from the beginning.
Part of her role involves explaining to patients and their family members how to live with mechanical cardiac-assist device technology in their daily lives.
"LVAD technology has greatly improved since our program began," Marnie says. "The size of the blood pumps which are implanted are much smaller and more comfortable for the patients.
"The old devices were loud and you could hear the pumps when the patient was in the same room as you," she says. "The new LVAD pumps are quiet and not audible unless you listen to the patient's chest with a stethoscope.
"They are much more reliable and are less likely to malfunction now than in the past when we first started implanting LVADs. In the past we would see the device start to fail after two years."
To commemorate the five-year milestone, Gurdip's wife, Jasraj Bhatia, brought in snacks and desserts for the medical team that saved her husband's life.
The impromptu celebration happened during Gurdip's clinic appointment at PMCC on Jan. 21 of this year, which is also the couple's 40th wedding anniversary.
"There was a time, I did not want to talk about it," says Jasraj Bhatia. "Now I want people to know. They need to have the strength.
"Even the smallest symptoms, you need to be alert."
