In a Canadian first, thoracic surgeons at TGH used a robotic surgical system to treat early-stage lung cancer by removing the cancer, along with a lobe of the lung. The use of this system improves outcomes after surgery and will expand the numbers of patients who can benefit from this type of minimally invasive surgical treatment.
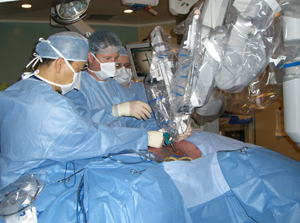 In their pioneering work, a team of surgeons led by Dr. Kazuhiro Yasufuku, Director of the Interventional Thoracic Surgical Program at TGH, and Dr. Tom Waddell, thoracic surgeon and Head of the Division of Thoracic Surgery, performed a robotic surgery on a 78-year-old man with a tumour the size of a penny in his lung's upper right lobe. The surgery was performed at TGH, as part of the Princess Margaret Cancer Program.
In their pioneering work, a team of surgeons led by Dr. Kazuhiro Yasufuku, Director of the Interventional Thoracic Surgical Program at TGH, and Dr. Tom Waddell, thoracic surgeon and Head of the Division of Thoracic Surgery, performed a robotic surgery on a 78-year-old man with a tumour the size of a penny in his lung's upper right lobe. The surgery was performed at TGH, as part of the Princess Margaret Cancer Program.
"More than 70% of lung cancers have a good chance of being cured, if they are treated early enough, so we have brought together a team of surgeon-scientists, who use and further develop the latest technology to try and change lung cancer's horrible statistics, " says Dr. Yasufuku, adding that the future of treatment belongs to robotics since it can incorporate different imaging modalities which will guide surgeons to perform surgery more safely, and possibly more precisely, something that is not possible with other techniques.
Dr. Yasufuku, one of the most internationally respected thoracic surgeons with expertise in minimally invasive thoracic surgery and diagnostic procedures, was recruited from Tokyo, Japan to set up a unique Interventional Thoracic Surgical Program at TGH, which includes the development of novel technology and a surgical suite to improve the current ways of diagnosing and treating lung cancer.
The day after his robotic surgery on October 20, 2011, Stanley Skorpid, 78, was able to get out of bed, and eat cornflakes for breakfast. On the third day, Stanley was impatiently walking the hospital hallways, and on the fifth day, he was glad to be going home. He is now back at work as a concierge, and continues to walk his German shepherd dog, Skor, about one mile to the lake close to his home.
On his second post-operative check-up today, Stanley remains cancer-free. "I'm still here," he says happily, "I'm feeling good."
Many centres would not consider surgery for someone of Stanley's age, points out Dr. Yasufuku, noting that the use of the robotic system contributed to Stanley's early recovery, along with minimal complications and pain, and a better quality of life.
Surgeons at TGH have since performed six more successful surgeries with the robotic technique on patients with lung cancer. The patients typically have shorter hospital stays, less pain, easier recoveries, less blood loss and scarring than as if they had been operated on with open-incision surgery.
"The robot becomes your hands, it augments what your hands can do," explains Dr. Yasufuku. "It's so easy for your hands to move much more finely right inside the patient. They can get in really deep."
To date, robotic surgery has most often been used for prostate and gynecological surgeries. It is now being used in several U.S. and European centres, and at TGH, as a useful technique in treating lung cancer. Studies in the 2011 Journal of Thoracic and Cardiovascular Surgery have shown that it is a safe procedure, and results in lower morbidity, such as blood loss, risk of infection, lower mortality, shorter hospital stays, and better quality of life than rib-and nerve-sparing thoracotomy.
In 2008, the Muzzo Family Charitable Foundation made a very generous pledge gift of $5,000,000 through the Princess Margaret Hospital Foundation to purchase the Da Vinci robot and to provide related program funding. This gift enabled the robotics program to begin and PMHF and UHN are very grateful to the Muzzo family for their ongoing support and keen interest in the program's development.
"We are proud to be able to contribute to such a leading edge technology with the potential to directly impact a patient's recovery in a very difficult time," said Marc Muzzo.
For doctors wishing to refer patients for robotic surgery consideration, please contact the University Health Network Lung Cancer Rapid Assessment and Management Program (LungRAMP):
Hotline: 1- 877-Lung911 (877- 586-4911) or
Fax: 416-340-3353 or
Email:
lung911@uhn.ca.
