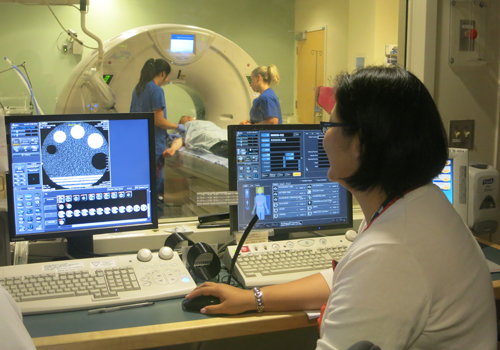
Under the care of a Medical Radiation Technologist from the Joint Department of Medical Imaging (JDMI), stroke patients undergo a series of scans to provide the medical team with more information about their stroke and how it’s affecting their brain. (Photo: UHN)
June is Stroke Awareness Month. On June 10, join the Krembil Neuroscience Centre's Stroke Program in the atrium of Toronto Western Hospital between 10 and 2 to learn about the warning signs of stroke and how to prevent them.
Relu Wiegner, stroke nurse with the Krembil Neuroscience Centre's stroke program, had received a call from Emergency Medical Services (EMS). They were on route to Toronto Western Hospital with a patient suffering a stroke.
Wiegner activated the fan out pager, simultaneously notifying all members of the on-call stroke team that a code stroke was on the way. In an instant, the on-call stroke neurologist, resident, and interventional neuroradiologist were notified to head to the Emergency Department (ED) to meet the patient on arrival.
When it comes to stroke, time is brain, and every minute counts in order to stop and reverse the damage occurring in the brain.
A quick response
Chris Kenalty had been out for dinner when his symptoms – a drooping face and drooling – had started, and he was quickly losing his faculties.
Dr. Leanne Casaubon, neurologist and the on-call stroke specialist that night, met the ambulance and directed the paramedics to triage. In less than 15 minutes, Kenalty was registered and whisked off for several brain and blood vessel scans to determine what type of stroke he was having. For instance, were the vessels in his brain blocked or was he experiencing bleeding in the brain?
"Things need to happen quickly but they also need to be done efficiently," says Casaubon. "The Stroke Team at TWH is well organized and we all know our roles to make this process go as smoothly as possible."
Although time is precious, determining the right course of treatment is paramount. The standard drug to treat stroke – tissue Plasminogen Activator (tPA) – cannot be used if a patient has bleeding in the brain or has recently had major surgery. It also cannot be given if a patient has been experiencing stroke symptoms for more than four and a half hours from the time they started.
Under the care of a Medical Radiation Technologist from the Joint Department of Medical Imaging (JDMI), Kenalty underwent a computerized tomography (CT) scan, a type of x-ray for the brain; a CT angiogram, to show detailed images of the blood vessels in his brain; and a CT perfusion which determines how much blood flow is getting to the brain tissue.
While Kenalty's scans were conducted, EMS briefed the Stroke Team with background details about the case. Information such as his medical history, current medications and vital signs were given for the team to make the best decision about Kenalty's care.
Paramedics also provided what is known as "last seen normal" time to pinpoint how long the patient was experiencing stroke symptoms before getting help.
After his scans, Casaubon and Wiegner used a stroke scale to examine Kenalty. This tool, a clinical exam used by healthcare providers, establishes how much a patient is impaired by a stroke based on the severity of his symptoms.
Determining a course of action
Kenalty's scan results showed a blood clot completely blocking a large vessel to the left side of his brain.
This information was taken with what was provided by paramedics, as well as the results of the stroke scale, to determine that tPA was the best course of action.
In less than an hour from his arrival time at TWH, Kenalty had been assessed and given the first part of his treatment. But the acute part of his care wasn't over yet.
tPA works to break down the blood clot that is blocking the blood vessel. After administering the tPA through an IV, the team monitors whether it's effective by conducting a stroke scale exam every 15 minutes.
However, sometimes tPA is unable to unblock a blood vessel. This is especially true when it is a larger brain blood vessel that is blocked, in which case additional treatments may be considered.
This was the case for Kenalty. The tPA alone was not likely to open his blocked blood vessel.
Based on his CT angiogram, the Stroke Team determined he was a candidate for an endovascular treatment (ET), a method to remove blood clots from the brain's blood vessels with a retrievable stent –a wire mesh tube-shaped device that is threaded into the blood vessel, closes around the clot and is then pulled out with the clot inside it.
Dr. Robert Willinsky, an interventional neuroradiologist, prepared to perform the procedure as Kenalty was wheeled over to the angiography suite.
Stay tuned: Visit UHN.ca tomorrow to find out the outcome of Chris Kenalty's treatment.
