Kim Rollins, 36, has spent two decades starving herself.
Her battle with a severe form of Anorexia Nervosa began at the age of 15. The Kitchener, Ont. native described it as her "worst nightmare".
She struggled daily with the urge to starve. Depression took hold. Anxiety over food – and the constant need to avoid it – consumed her. Exercise was a non-stop compulsion. In university, she ran the stairs in her dorm every day for up to three hours before going to class.
Broken bones
"I was just so depressed and something in me told me not to eat and just to exercise constantly, to the point of breaking my bones and hurting my heart." she said.
Over the years, Kim suffered several complications from her anorexia including a massive heart attack, two strokes, the onset of osteoporosis and several broken bones in her legs and feet due to constant exercising. Numerous attempts were made to get help, but nothing ever changed.
Most of her life was a never-ending cycle of treatment facilities, programs she could not complete and renewed attempts to get better through different treatment options.
"Treatment over the past 20 years has been a long, sad story for me," Kim said. "Being unable to complete the numerous programs I've been in took away all my hope."
'My life was a living hell'
Anorexia destroyed her social life, too. Although Kim managed to stay in university, she led an empty life.
"I really didn't have the life experiences that most women in their 20s do. I didn't have any friends, I was very isolated, I was never in a relationship. My life was a living hell, completely consumed by my illness," she said.
By 2005, at the age of 28, Kim's struggle with anorexia had reached its most dire point. At a height of 5 feet 2 inches, her weight had dropped to 71 pounds.
A reason to hope
In 2011, after being unable to complete yet another treatment program, Kim heard about a study involving anorexia patients. It was unlike any treatment she'd ever heard of before. It involved brain surgery – and she signed up immediately.
The study, led by Dr. Andres Lozano at UHN's Krembil Neuroscience Centre at Toronto Western Hospital, involved a procedure called Deep Brain Stimulation (DBS).
Since research shows that brain circuits associated with mood, anxiety, reward and body perception differ between anorexia patients and those who are healthy, DBS involves targeting those brain circuits.
In the surgery, electrodes are implanted in the brain to send signals to dysfunctional neurons that are linked to emotion. These signals decrease the activity of the dysfunctional brain circuits, thus, weakening the compulsive urges of anorexia patients.
Patients speak during surgery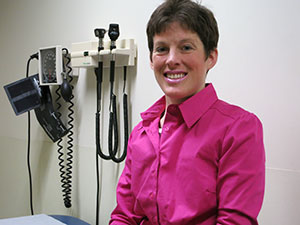
Patients were awake during the procedure and spoke out when brain circuits were stimulated, signalling to doctors that they'd found the right neurons to target. For example, in Kim's case, implanting the electrodes led her to describe that things felt "brighter" and the intensity of her fear lessened.
Once implanted, the electrodes were connected to an implanted pulse generator below the right collarbone, similar to a heart pacemaker.
The procedure was performed on six study participants. Nine-months after the surgery, three of the six patients – including Kim – gained weight.
Photo: Today, post-DBS surgery, Kim Rollins is happier and healthier. (Photo: courtesy of Kim Rollins)
For these patients, this was the longest period of sustained weight gain since the onset of their illness. Furthermore, four of the six patients also experienced simultaneous changes in mood, anxiety and control over emotional responses, such as urges to binge and purge. As a result of these changes, Kim and another study participant were able to complete an inpatient eating disorders program for the first time.
Medical experts pleased
For Dr. Lozano and his team, the results are extremely encouraging.
"We are truly ushering in a new of era of understanding of the brain and the role it can play in certain neurological disorders," said Dr. Lozano, a leading international expert in the DBS field. "By pinpointing and correcting the precise circuits in the brain associated with the symptoms of some of these conditions, we are finding additional options to treat these illnesses."
The impact of the research study may not only provide an additional therapy option in the future for patients suffering from severe anorexia, but it also furthers practitioners' understanding of anorexia and the factors that cause it to be persistent.
"Eating disorders have the highest death rate of any mental illness and more and more women are dying from anorexia," said Dr. Blake Woodside, medical director of Canada's largest eating disorders program at Toronto General Hospital. "Any treatment that could potentially change the natural course of this illness is not just offering hope but saving the lives for those that suffer from the extreme form of this condition."
A new life
For Kim, the procedure has made a world of difference. She is healthier, happier and is living a completely different life.
Recently, she experienced the simple pleasure of having a piece of birthday cake to celebrate her nephew's birthday with her family, an event she would normally have shunned by not eating and shutting herself up in her room.
"From the depths of my anorexia, I never thought this would be possible," she said. "This procedure gave me new life, new hope. I am moving on with my life in a positive direction and making plans for my future that would never have been possible before the surgery."
Related
Press release: Deep Brain Stimulation shows promise for patients with chronic, treatment resistant Anorexia Nervosa
