Research into improving cancer treatments is helping patients live longer, but as with many diseases, treatments and medications come with a host of side effects that can affect patients' quality of life.
Helping patients self-manage symptoms associated with cancer treatment is the focus of Dr. Doris Howell's recent study, which is looking at the use of a smart phone-based system to help patients monitor and manage their symptoms at home.
The research team has customized the system developed in the United Kingdom for use in Canada with patients undergoing chemotherapy treatment.
"Cancer has lagged all of the other chronic diseases for standardizing self-management education and support," says Dr. Howell, Senior Scientist at Princess Margaret Cancer Centre.
"There have been huge efforts across Canada for diseases like arthritis and diabetes, but only more recently has there been a push towards developing standards and systematic approaches to self-management support for cancer in the province of Ontario."
The randomized control trial has 44 patients using the phone-based system and the same number receiving standard care. Patients using the phone device can report the symptoms they are experiencing and their scores for the severity of their symptoms in real-time.
The system will automate self-care advice to the patient and outline actions they can take to manage those symptom issues. At the same time, if the symptoms are severe, it will alert a designated clinician on the patient's care team.
If the clinician receives a yellow alert, they should follow up with the patient within four hours, and if it is a red alert, within 30 minutes.
"It's a smart system in the sense that patients will answer a first question about the particular symptom problem, and if it's concerning, the system will ask follow up questions and integrate responses to estimate risk," Dr. Howell explains.
"So if a patient has severe vomiting, for example, it will ask additional questions to determine if there are signs of dehydration."
When the clinician goes into the system, it will triage them through those additional questions to allow them to determine whether to advise the patient on specific actions they can take to manage the symptom, escalate it to the physician, or whether a visit to the emergency department is warranted.
Empowering patients
While teaching patients how to manage their symptoms is part of the standard of care at the Princess Margaret, Dr. Howell says the process can be overwhelming for patients who have just learned they have the disease.
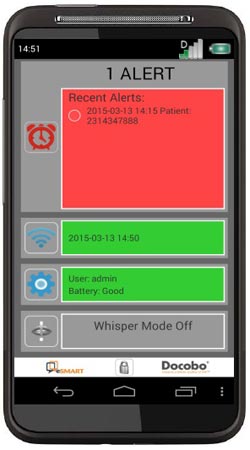
The patients’ care teams also receives a device to get alerts when reported symptoms are severe. (Photo: Courtesy Dr. Doris Howell)
"It can be tough for patients when they're newly diagnosed and we teach them about all of these side effects in one session, and give them multiple pamphlets and reading materials – it's hugely challenging to absorb all that information," Dr. Howell says.
"With the mobile symptom monitoring and management system, patients have immediate access to a self-care library to read more and get background information about the symptom, and they learn very specific actions and strategies they should be taking in the moment when they're experiencing the symptom."
Dr. Howell and her team will be studying the effects of the system on patients in terms of reduction of symptom severity and better quality of life. They will also observe how clinicians integrate this new approach into their daily practice, and look at barriers to using the system for both clinicians and patients.
Similar systems used in the U.S. have shown that it can reduce urgent care use and has shown better survival rates in patients when clinicians are alerted.
Dr. Howell says the study is important for shifting care delivery from being reactive to proactive and fosters better patient engagement in disease management.
"It's an early detection and intervention approach to prevent these symptoms from getting serious and minimize consequences instead of responding to them after they already occur."
She adds that putting symptom management in the hands of patients is empowering and demonstrates how patient care is evolving.
"This kind of technology is where the future is going in terms of how we're going to reach patients on a wider scale because they're not going to come back to our organizations to get care on an ongoing basis," Dr. Howell says.
"So this is really looking at empowering patients and actually integrating better personalized self-management support at the point of care."
Dr. Howell, who is also the RBC Chair in Oncology Nursing Research and Education, has made significant contributions to advancing the quality of personalized cancer symptom management to reduce symptom burden and optimize health. This has been achieved through research that has focused on testing health service innovations to capture the "whole person" impact of cancer and treatment using self-report measures for better patient management in clinical care and to engage patients' in self-management of cancer symptoms to optimize health recovery during and after cancer treatment.
