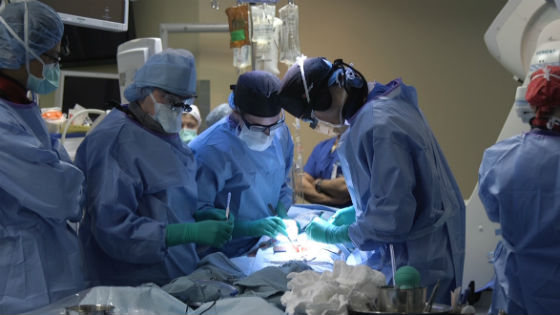
A multi-disciplinary medical team performs a complex vascular surgery procedure at the Peter Munk Cardiac Centre, involving physician expertise in cardiac, vascular and radiology, among other specialties. (Photo: PMCC)
Steven Stamkos, a star player in the National Hockey League, was to undergo a vascular procedure in Florida today. The Tampa Bay Lightning forward, who hails from Markham, Ont., was discovered to have a blood clot in his right arm, diagnosed as Venous Thoracic Outlet Syndrome by doctors in Florida.
The Peter Munk Cardiac Centre (PMCC) is a leading centre in Canada for treatment of this condition.
PMCC vascular surgeons, Dr. George Oreopoulos and Dr. Graham Roche-Nagle, answer some common questions about this rare condition.
What is the condition called?
Venous Thoracic Outlet Syndrome (VTOS) is also known as Effort Vein Thrombosis and Paget–Schroetter Syndrome.
How common is Venous Thoracic Outlet Syndrome?
It is a rare condition. The general incidence of UEDVT remains low (approximately two per 100,000 people annually.) It is regarded as the most common vascular condition among athletes.
How many cases does PMCC see on average a year of this?
15-20 cases per year from all over Ontario
Related to this story
Dr. Graham Roche-Nagle on Sportsnet
What are the symptoms of Venous Thoracic Outlet Syndrome?
Patients typically present with an acutely swollen arm and hand with heaviness and sometimes tingling/numbness. This is often accompanied by a bluish discolouration of the hand (cyanosis) and some prominent superficial veins across the shoulder and upper chest on the same side.
This presentation often occurs after especially strenuous or unusually vigorous physical activity and is often called an "effort thrombosis."
 Dr. George Oreopoulos, vascular surgeon, Peter Munk Cardiac Centre, says Venous Thoracic Outlet Syndrome is a rare disorder which in some cases can be fatal without proper diagnosis and appropriate medical treatment, which includes the use of blood thinners.(Photo: PMCC)
Dr. George Oreopoulos, vascular surgeon, Peter Munk Cardiac Centre, says Venous Thoracic Outlet Syndrome is a rare disorder which in some cases can be fatal without proper diagnosis and appropriate medical treatment, which includes the use of blood thinners.(Photo: PMCC)
Sometimes, patients may present to hospital with a pulmonary embolism with chest pain, an elevated heart rate and shortness of breath, making this a potentially life-threatening condition in a smaller percentage of patients.
Up to 12 percent of upper extremity Deep Vein Thrombosis may present with a pulmonary embolism.
Who is most afflicted?
It is a relatively infrequent disorder that occurs predominantly in young, otherwise healthy people who participate in repetitive upper-extremity activity. These movements are usually done during sport activities. We have treated baseball/rugby/volleyball/rowers/karate experts and other jobs painters etc., and sometimes gym enthusiasts.
How common is this condition in athletes?
Effort thrombosis is more common in athletes but exact numbers are hard to come by.
How is it diagnosed?
The diagnosis of an upper extremity DVT is suspected on clinical grounds and confirmed by ultrasound. Further testing using venography (x-ray of upper extremity veins with injection of x-ray dye, usually with the arm in multiple different positions confirms the diagnosis.)
 Dr. Graham Roche-Nagle, vascular surgeon is part of a seven-member Vascular Surger team at the Peter Munk Cardiac Centre, which see about 20 cases a year of patients diagnosed with Venous Thoracic Outlet Syndrome, commonly found in athletes.(Photo: PMCC)
Dr. Graham Roche-Nagle, vascular surgeon is part of a seven-member Vascular Surger team at the Peter Munk Cardiac Centre, which see about 20 cases a year of patients diagnosed with Venous Thoracic Outlet Syndrome, commonly found in athletes.(Photo: PMCC)
Most common treatment options?
Frontline treatment is anticoagulation (blood thinners). This alone may be inadequate for the prevention of long-term symptoms in very active or high- performance individuals. Clearance of the blood clot by catheter-directed thrombolysis followed by surgical removal of part of the first rib helps to prevent recurrent blood clots and disabling symptoms in these individuals.
What specific expertise does PMCC have that makes it a lead centre for treatment?
The PMCC has a multidisciplinary team that facilitates all aspects of treatment of VTOS in a single centre. PMCC has a multidisciplinary TOS clinic where physicians see patients with the help of a physiotherapist with special expertise in this area. Patients are seen in clinic or in the emergency room for more urgent cases and are treated initially in Interventional Radiology when catheter-directed thrombolysis is required. When appropriate, patients are operated on by the Vascular Surgery team for first rib resection. Anticoagulation is often managed with the assistance of experts from UHN's Thrombosis clinic.
Typical prognosis for these patients?
The condition can be fatal or cause a potentially fatal complication. Timely, accurate clinical recognition of the signs and symptoms of it is necessary to facilitate appropriate medical referral and treatment. Most individuals but not all return to their previous activities after an additional period of anticoagulation while the vein heals.
What does recovery usually involve?
Younger individuals tend to recover over a period of two to three months and can return to a relatively normal life without blood thinners (anticoagulation).
